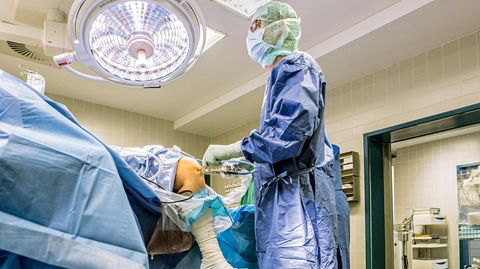
Feature Image of an Unloader Knee Brace sourced from:
https://www.ossur.com/oa-solutions/research
An earlier blog post discussed autologous cartilage transplantation for defective knee cartilage:
Transplantation of One’s Own Knee Cartilage – Is this ‘The Bee’s Knees’ for Painful Knees?
Dear Pain Matters readers,
Introduction
Here’s a sobering thought:
The biggest cause of disability in the U.S. is osteoarthritis (OA), with the medial compartment (i.e. inside part) of the knee being most commonly affected (Vincent et al, 2012).
Most medical experts state that due to its avascular and aneural nature, articular cartilage cannot regenerate in vivo, especially during persistent inflammation following trauma or injury to cartilage (Huey et al, 2012).
Other researchers believe that knee cartilage is able to regenerate in vivo, but only in a chondrocyte-friendly environment. This would require nil ‘bone-on-bone’, nil localised inflammation, reduced or nil knee pain, healthy synovial fluid in the articular cavity and highly vascularised underlying subchondral bone (Lyu et al, 2011; Tiku & Sabaawy, 2015).
In the absence of effective treatment, deterioration of the knee joint may continue until finally, most if not all of the cartilage tissue is worn out and arthritic. At this stage, total knee replacement (arthroplasty) may be the only option left.
As such, a proactive approach to knee health is important. This is because a painful knee joint will either get better or worse. Nothing stays the same.
The good news is that treatments do exist whereby ‘bone-on-bone’ knee pain may be reduced and even eliminated altogether in some instances. These include non-weight-bearing exercises such as swimming, aquatic exercises and cycling. Wearing a fitted unloader knee brace may also be helpful.
Unloader Knee Braces
Regardless whether cartilage is able to regenerate in vivo or not, fitted unloader (or offloader) knee braces may offer benefits including relief from knee pain, increased knee stability and enhanced mobility.
By shifting the load-bearing weight toward the lateral (outside) part of the knee, the brace may help increase the gap between the femur bone and the medial (inside) part of the tibia. (The lateral side is usually the ‘good’ side of the knee in patients with medial knee OA.) This gap reduces ‘bone-on-bone’ and hence leads to reduced inflammation in an OA-affected knee joint.
An unloader brace-induced gap can promote a chondrocyte- and mesenchymal stem cell**-friendly environment that might lead to cartilage regeneration.
On the other hand, the absence of normal cartilage or the absence of a compensatory unloader knee brace may lead to ‘bone-on-bone’ between the connecting bones in the knee joint. Without a gap between the bones, further knee joint deterioration occurs until finally, ‘bone-on-bone’ knee pain results. Walking may become unbearable unless the patient opts for an unloader knee brace (if beneficial) or has total knee replacement.
Thus, OA knee patients may benefit from a prescription for a fitted unloader brace for walking, hiking and other light load-bearing activities. Wearing an unloader brace may relieve knee pain, swelling and other symptoms as well as prevent further deterioration in the defective knee cartilage.
For some OA patients, wearing an unloader knee brace may be all that is required ‘to keep going’ and hence, defer costly total knee replacement indefinitely (Mistry et al, 2018).
A Friend’s Unloader Knee Brace Story
Several years ago, I kept running into a nice lady named ‘Jane’ (70) in a nearby park. Appearing fit and trim while walking her dog, Jane always wore her unloader knee brace.
One day while chatting, I asked her why she wore a knee brace. Jane replied that sadly, one of her knees was now ‘bone-on-bone’. Consequently, Jane found walking very painful without her knee brace. She added that luckily, she finally found pain relief while walking her dog as long as she wore her unloader brace.
It all started when Jane’s orthopaedic surgeon stated that she needed total knee replacement due to ‘bone-on-bone’ knee pain. When the surgeon proposed a date for this surgery, she realised that the date for surgery conflicted with a long-planned golfing holiday with her husband. Since there were no other times available for surgery, her surgeon prescribed an unloader knee brace until her return.
From Jane’s perspective, this was the best treatment ever for her knee pain. Jane was finally able to walk her dog for kilometres at a time without pain. She was able to manage without a knee brace in her own house.
The story does not end here. It only gets even better!
A year later, I saw Jane outside of her house while walking past. She was not wearing her knee brace. After a chat, I asked her how her knee was doing.
Jane’s answer took me by complete surprise. Jane told me that she had cancelled her knee surgery indefinitely. This was because she no longer needed her knee brace while walking her dog.
Lost for words, I asked, ‘Why not?’
Jane replied that recently, her small dog had run out of the house to chase another dog down the road. Worried that her dog might get hit by a car and in a hurry to catch up to her dog, Jane forgot to put on her knee brace. Instead, she ran as quickly as she could to chase down her beloved dog. When Jane finally did catch up, she was relieved to find her dog safe and well.
On their way back home, Jane noticed something weird. She was not wearing her unloader knee brace. Even stranger, Jane had nil knee pain despite running after her dog without her knee brace!
‘How is this even possible?’, she asked herself.
In Jane’s opinion, her knee cartilage may have regrown due to her wearing an unloader brace daily while walking her dog. Jane would never have realised that her cartilage had regenerated if her dog hadn’t suddenly run out of their house that day. This is because normally, Jane would never walk her dog without her knee brace.
Jane joked that her brace must have given her knee a much-needed ‘knee holiday’.
Thanks to Jane’s brace, her knee no longer endured ‘bone-on-bone’ pain while walking her dog. This led to reduced irritation and inflammation as well as possible cartilage regeneration.
I thought it was fantastic that in lieu of total knee replacement, Jane was prescribed an unloader knee brace. This knee brace enabled Jane to take long walks with her dog every day without knee pain. Furthermore, Jane no longer needed her knee brace one year later.
Jane’s knee cartilage may have regrown thanks to the ‘knee holiday’ that her brace offered. Despite no longer wearing her brace while walking her dog, Jane no longer had any ‘bone-on-bone’ knee pain.
Just as a dog can be a man’s (or a woman’s) best friend, an unloader knee brace may be an OA knee’s best friend.
An unloader knee brace was the only thing that Jane needed for ‘bone-on-bone’ knee pain. And thanks to her misadventure with her dog, she found out that she no longer needed a knee brace one year later!
After listening to this incredible story, I was happy that Jane was able to defer total knee replacement surgery indefinitely.
Some questions:
What would have happened if Jane had done nothing at all? In other words, what if Jane was not prescribed an unloader knee brace and had not considered total knee replacement surgery?
I suspect that if Jane had done nothing at all, her knee may have deteriorated even further.
A ‘bad’ knee sometimes degenerates to the point where walking becomes impossible without a cane, walker or wheelchair – until joint replacement.
As such, doing nothing is not usually a good option. One needs to be proactive in the care of one’s own health including the health of one’s knees.
If one has painful knees, one should first seek out less invasive knee treatments. This may include an unloader knee brace, physiotherapy, non-load-bearing exercises (e.g. swimming and other aquatic exercises, cycling), a healthier diet, losing weight and/or autologous cartilage transplantation (see link at top).
If conservative treatment(s) are pursued in a timely manner, it may be possible to save a knee joint, hence defer total knee replacement indefinitely.
Finally, what exactly went on inside Jane’s knee while she wore her unloader knee brace??
To try to answer this question, I explored the science behind Jane’s knee recovery. This is what I found:
The Science Behind Jane’s Knee Recovery

Image of unloader (valgus) knee brace for medial knee OA sourced from:
https://www.sciencedirect.com/science/article/pii/S1877065715000561
Overview
A properly fitted unloader knee brace may help keep a patient on his/her feet while slowing or stopping further ‘bone-on-bone’ deterioration of the knee joint. This may lead to reduced knee pain and increased mobility.
A fitted unloader brace is designed to alleviate the mechanical strain on the defective load-bearing cartilage. As such, cartilage regeneration in vivo may occur in some OA patients after wearing an unloader brace for many months.
Whether cartilage regenerates or not is not the biggest issue. It may even be impossible in most OA knee patients.
A greater concern is whether reduced (or nil) ‘bone-on-bone’ pain and increased mobility results while wearing an unloader knee brace during weight-bearing activity. If yes, ongoing use of this brace is warranted as long as desired.
Some OA patients may prefer a non-invasive unloader brace over total knee replacement surgery, osteotomy, pain medication including knee injections or doing nothing at all.
Others may not qualify for total knee replacement surgery due to being younger than 50 or older than 80. As such, patients aged less than 50 with a severely arthritic and painful knee may benefit from an unloader brace.
Patients with unicompartment knee OA* may benefit from unloader braces that may decrease (or eliminate) pain, enhance knee function and perhaps even slow OA progression.
Knee Joint Distraction Therapy
Knee joint distraction therapy involves applying an external force to the knee joint via an unloader knee brace (preferably, not via an invasive external fixation frame). Such a brace can be adjusted to exert external forces to either the inside or the outside of the knee, depending on which side is affected by OA.
Pain relief and reduced swelling often occur following distraction therapy of the arthritic, load-bearing part of the knee. This therapy may either shift load-bearing weight from the medial (i.e. inside; valgus) compartment to the lateral (i.e. outside; varus) compartment of the knee, or vice versa (depending on which side is affected by arthritis).
In other words, knee joint distraction therapy via an unloader brace shifts the weight away from the arthritic knee compartment including degenerated cartilage and toward the ‘good’ side of the knee joint.
Furthermore, an unloader brace may improve the overall alignment of the knee joint.
Finally, an unloader brace may alleviate the ‘bone-on-bone’ pain in the knee by slightly increasing the gap between the femur bone and tibia bone on the arthritic side of the knee joint.
For example, a knee unloader brace with valgus adjustments may be prescribed for medial unicompartment knee OA. This may be desirable before considering other more invasive surgical options such as osteotomy or arthroplasty (Ramsey & Russell, 2009).
Summary
In summary, an unloader brace-induced chondrocyte-friendly knee joint may result. This may lead to reduced or nil pain and swelling, increased mobility and perhaps even cartilage regeneration (Callaghan et al, 2015; Kirane et al; Lafeber et al, 2006; Lee et al, 2017; Mastbergen, 2013; Ornetti et al, 2015; Ramsey & Russell, 2009; Thoumie et al, 2018; Tiku & Sabaawy, 2015; van der Woude et al, 2016a; van der Woude et al, 2016b; van der Woude et al, 2017; Verkerke et al, 2014).
One last question:
Is cartilage regeneration more likely to occur if both:
- An unloader knee brace is worn; and
- Autologous cartilage transplantation is done (where appropriate)?
(The latter is discussed here:
Transplantation of One’s Own Knee Cartilage – Is this ‘The Bee’s Knees’ for Painful Knees?)
Unloader Knee Brace Patient Stories
Dermott Brereton

Dermott Brereton
Source: https://www.unloader.com.au/knee-pain/dermott-brereton
Former Australian Football League Player, Dermott Brereton (54), endured painful OA in his left knee for more than 30 years after tearing his cartilage during a game in 1984, aged only 19.
Following unsuccessful knee surgery, his injured cartilage had to be removed a year later. Sadly, Dermott was left with ‘bone-on-bone’ knee pain. Quoting Dermott,
‘It’s been painful to walk on ever since and can be excruciating when the pain’s most acute.’
Dermott continued,
‘… People ask me what’s it like, ‘bone-on-bone’ [pain] … I describe it as biting on a bit of tin foil. That’s what it is in between the 2 [bones] of your knee …
Rather than having invasive total knee replacement surgery, Dermott decided to wear the Unloader One Lite knee brace … and he hasn’t looked back since!
Weighing only 296g and featuring Össur’s 3-Point Leverage System, the Unloader One Lite knee brace is the lightest unloader knee brace currently available.
Dermott has worn this unloader knee brace for several months with significant success. In his words,
‘… The Unloader [knee brace] … pulls those 2 sensitive points apart …
More details are available in the 1-minute YouTube video as well as in the following links:
https://www.unloader.com.au/knee-pain/user-stories
https://www.unloader.com.au/knee-pain/dermott-brereton
Other Unloader Knee Brace Stories
Quoting a
61-year old retired male professional,
‘I have one of these [unloader knee] braces and I wish I had this 3 years ago. I now ride my Trike all over New Zealand.’
For additional positive unloader knee brace stories, see YouTube videos and testimonials by OA patients including by:
- ‘Tony’, a father of 2 girls;
- A 45-year old male who enjoys kite surfing;
- 9 other men including fathers;
- A female hiker (age unknown);
- An Asian woman who practices yoga.
- A female (61); and
- A knee pain patient (gender unknown).
For ‘Stories From Unloader Brace Users’, click here:
https://www.unloader.com.au/knee-pain/user-stories
Summary
Osteoarthritis knee patients should wear fitted unloader knee braces before contemplating total knee replacement surgery.
One never knows … there may be some life left in many knees, thanks to fitted unloader knee braces.
Key
* Unicompartment knee OA involves degeneration of the knee joint including defective articular cartilage. The medial part of the knee joint is more commonly affected than the lateral part.
** Mesenchymal stem cells are the progenitor of chondrocytes. They originate and reside in peri-articular bone marrow and subchondral bone. Mesenchymal stem cells are also present in cartilage, synovium, synovial fluid, infrapatellar/sub-synovial fat pad and adipose tissue (Mastbergen, 2013; McGonagle et al, 2017).
References
MEDIA
(1A) Global Orthopaedics leader Össur announces AFL Legend Dermott Brereton as ambassador for revolutionary osteoarthritis knee braces – Unloader One Lite. Össur.
(1B) Stories From Unloader Brace Users. Össur.
https://www.unloader.com.au/knee-pain/dermott-brereton
(2A) Bedard, Richard. Knee Cartilage Repair: How One Patient Proved His Doctors Wrong. Huffpost (16 Aug 2011).
https://www.huffpost.com/entry/knee-cartilage-repair_n_876946
(2B) Bedard, Richard. Saving My Knees: How I Proved My Doctors Wrong and Beat Chronic Knee Pain. Pages 1-208.
PEER-REVIEWED PAPERS
IS CARTILAGE REGENERATION POSSIBLE IN VIVO?
(1A) Lyu et al. Knee Health Promotion Option for Osteoarthritic Knee: Cartilage Regeneration is Possible, Osteoarthritis – Diagnosis, Treatment and Surgery, Prof. Qian Chen (Ed.) (2012).
ISBN: 978-953-51-0168-0, InTech,
http://www.intechopen.com/books/osteoarthritis-diagnosis-treatment-and-surgery/knee-health-promotion- option-for-osteoarthritic-knee-cartilage-regeneration-is-possible
(1B) Lyu et al. Arthroscopic cartilage regeneration facilitating procedure for osteoarthritic knee. MC Musculoskeletal Disorders (21 Nov 2012); 13: 226.
https://doi.org/10.1186/1471-2474-13-226
https://bmcmusculoskeletdisord.biomedcentral.com/articles/10.1186/1471-2474-13-226
(1C) Other papers and thoughts by Lyu et al on whether cartilage regeneration could occur by itself, and in vivo:
https://www.researchgate.net/post/Is_it_possible_that_cartilage_regeneration_could_happen_by_itself
(1D) Ding et al. Natural History of Knee Cartilage Defects and Factors Affecting Change. (27 March 2006)
https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/410037
JOINT DISTRACTION THERAPY FOR OSTEOARTHRITIS USING UNLOADER KNEE BRACE (NOT INVASIVE EXTERNAL FIXATION FRAME)
(2A) Tiku & Sabaawy. Cartilage regeneration for treatment of osteoarthritis: a paradigm for nonsurgical intervention. Ther Adv Musculoskelet Dis (2015); 7(3): 76-87.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4426098/pdf/10.1177_1759720X15576866.pdf
(2B) Callaghan et al. (2015) A randomised trial of a brace for patellofemoral osteoarthritis targeting knee pain and bone marrow lesions. Ann Rheum Dis (16 January 2015); 74(6): 1164–1170.
doi 10.1136/annrheumdis-2014-206376
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4771926/
(2C) Lafeber et al. Unloading joints to treat osteoarthritis, including joint distraction. Curr Opin Rheumatol (2006); 18(5): 519–525.
https://www.ncbi.nlm.nih.gov/pubmed/16896294
(2D) Verkerke et al. Knee Orthosis for Cartilage Repair. Knee Orthosis for Cartilage Repair (October 2014); 32-33.
https://www.researchgate.net/publication/270879215_Knee_Orthosis_for_Cartilage_Repair
(2E) Ramsey & Russell. Unloader Braces for Medial Compartment Knee Osteoarthritis. Sports Health (Sept 2009); 1(5): 416–426.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3445170/
(2F) van der Woude et al. Five-Year Follow-up of Knee Joint Distraction: Clinical Benefit and Cartilaginous Tissue Repair in an Open Uncontrolled Prospective Study. Cartilage (July 2017); 8(3): 263–271.
(2G) van der Woude et al. Knee Joint Distraction Compared to Total Knee Arthroplasty for Treatment of End Stage Osteoarthritis: Simulating Long-Term Outcomes and Cost-Effectiveness. PLoS One(12 May 2016); 11(5): e0155524.
(2H) van der Woude et al. #885 – Six Weeks of Knee Joint Distraction: Sufficient for Cartilage Tissue Repair. Abstracts / Osteoarthritis and Cartilage 24 (2016); S63eS534
https://www.oarsijournal.com/article/S1063-4584(16)00958-4/pdf
(2J) Mastbergen, S. SP0166 Joint Distraction and Cartilage Regeneration – What is the Basis for Structural Repair? Ann Rheum Dis (2013); 72(Suppl 3).http://dx.doi.org/10.1136/annrheumdis-2013-eular.166
https://ard.bmj.com/content/72/Suppl_3/A38.2
(2K) McGonagle et al. Native joint-resident mesenchymal stem cells for cartilage repair in osteoarthritis. Nat Rev Rheumatol (Dec 2017); 13(12): 719-730.
doi 10.1038/nrrheum.2017.182.
https://www.ncbi.nlm.nih.gov/pubmed/29118440
(2L) Centeno, CJ. Can an Aggressive Knee Surgical Implant Regrow Cartilage? Regenexx (5 Sept 2013).
https://www.regenexx.com/blog/regrow-cartilage/
(2M) Intema et al. Tissue structure modification in knee osteoarthritis by use of joint distraction: an open 1-year pilot study. Ann Rheum Dis (12 May 2011); 70: 1441–1446.
doi 10.1136/ard.2010.142364
(2P) Mistry et al. An Update on Unloading Knee Braces in the Treatment of Unicompartmental Knee Osteoarthritis from the Last 10 Years: A Literature Review. Surg J (N Y) (2 Jul 2018); 4(3): e110–e118.
(2Q) Lee et al. Unloading knee brace is a cost-effective method to bridge and delay surgery in unicompartmental knee arthritis. BMJ Open Sport Exerc Med (31 Jan 2017); 2: e000195.
doi 10.1136/bmjsem-2016- 000195
https://bmjopensem.bmj.com/content/bmjosem/2/1/e000195.full.pdf
(2R) Thoumie et al. Effect of unloading brace treatment on pain and function in patients with symptomatic knee osteoarthritis: the ROTOR randomized clinical trial. Sci Rep (12 Jul 2018); 8(1): 10519.
doi 10.1038/s41598-018-28782-3
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6043544/pdf/41598_2018_Article_28782.pdf
(2S) Kirane et al. Offloading strategies for knee osteoarthritis. ler magazine (Sept 2010).
https://lermagazine.com/article/offloading-strategies-for-knee-osteoarthritis
OTHER
(3) Vincent et al. The Pathophysiology of Osteoarthritis: A Mechanical Perspective on the Knee Joint. PM R (May 2012); 4(5 Suppl): S3–S9.
doi:10.1016/j.pmrj.2012.01.020.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3635670/pdf/nihms449284.pdf
(4) Clinical Studies – 15 studies are listed here: